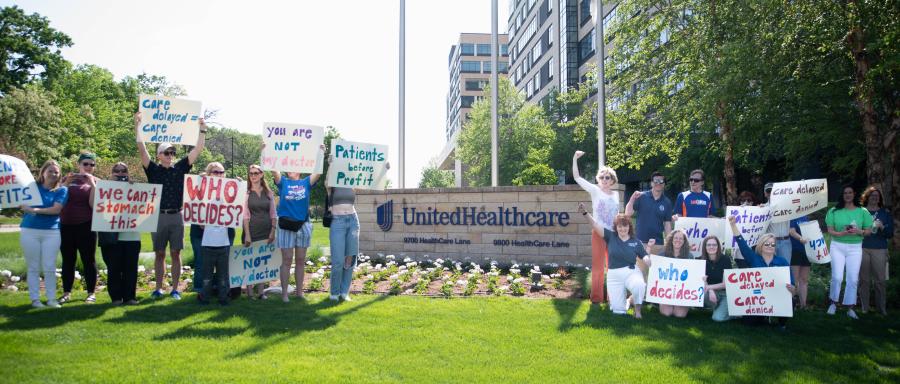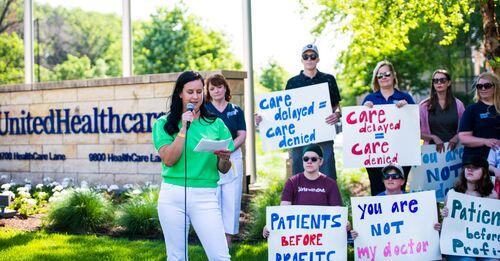We Can’t Stomach This: Foundation Holds Rally at UnitedHealthcare Headquarters Protesting Forthcoming Prior Authorization Policy
Published: June 14, 2023
On a warm Wednesday morning in late May, healthcare advocates from across the country joined the Foundation at United Healthcare’s headquarters in Minnetonka, Minnesota to protest a forthcoming policy that would have expanded prior authorization for most physician-prescribed endoscopy and colonoscopy procedures.
Holding signs reading “Patients Before Profits,” “We Can’t Stomach This,” “Care Delayed = Care Denied,” and “You Are Not My Doctor,” IBD patients, healthcare providers, and members of the colon cancer community convened at 9800 Healthcare Drive to voice their demands for immediate action Had it gone into effect, this prior authorization requirement would have disrupted time-sensitive care for millions of patients and created needless anxiety and delays for IBD and cancer patients.
Following the rally and significant backlash from the GI community, United Healthcare (UHC) delayed implementing this policy, which was slated to begin June 1. Close to 4,000 people in the Crohn’s and colitis community sent letters to UnitedHealthcare's CEO to urge him to stop harmful prior authorization requirements and to prevent further unnecessary delays of care for IBD patients. The Foundation was invited to meet with UHC to discuss the policy after the rally.
A Morning Of Advocacy
“Patients don’t measure results in dollars,” said Laura Wingate, Executive Vice President, Education, Support & Advocacy at the Foundation. “For them, results revolve around the invaluable impact of a new treatment that adds precious years to their lives. Results mean attaining a quality of life that enables them to actively participate in their community, pursue meaningful work, and experience the joy of being fully engaged. Results mean relief from the dilemma of having to choose between the financial burden of healthcare or feeding their family.”
Amber Backhaus, the incoming chair of the Crohn’s & Colitis Foundation’s Board of Trustees echoed these sentiments. “Let’s be honest- no one enjoys getting an endoscopy or colonoscopy,” she said. “But for patients with serious IBD issues, it is an essential step to managing their disease. Introducing these new barriers to care will result in patients missing tests and having to fight health insurance bureaucracy to receive the medical care their doctor says they need.”
To provide a glimpse into the potential ramifications of this proposed policy, Haley Mills, a Minneapolis resident who has lived with Crohn’s disease for the last two decades, shared her story:
“Over the years, I have had 20 surgeries and spent large chunks of my life in the hospital due to flare ups and complications of my disease. I have missed holidays, weddings, and other important days with my friends and family. There are long wait times to get in with GI providers. When I’m able to get into a provider, any delays from insurance companies for medications, colonoscopies, or endoscopies can mean the difference in ending up at the hospital again or healing at home. I’m really concerned that this new policy could mean significant delays in getting the colonoscopy I need to make a treatment decision, leading to rounds and rounds of appeals and ultimately worse outcomes for my disease.”
Dr. Dan Pambianco, President of the American College of Gastroenterology shed light on how the policy would place an undue burden on healthcare providers.
“This program is not only bad for patients, but there are also so many operational challenges that this creates that have been unanswered,” said Dr. Pambianco. “What that means is that my staff will be spending more time trying to get pre-authorizations. I will be spending more time on the phone getting peer-to-peer reviews than with patients. This will only leave us struggling, not improving our access to care.”
The Fight for Patient Access Continues
In response to the collective efforts of patients and professionals, UHC has instead introduced an Advance Notification Program for non-screening and nonemergent colonoscopies and endoscopies. The program is aimed at preparing for UHC's new "gold card" program scheduled for 2024. Under this planned program, physician practices with a high prior authorization approval rate will be exempt from prior authorization requirements for those services. Full details about the new program have not yet been provided by UHC, and they are still considering implementing prior authorization requirements with the “gold card” program in early 2024.
“While we are pleased that UnitedHealthcare seems to have heard our concerns, this policy still fails to take into account the unique needs of IBD patients,” said Laura Wingate “We need more details about the Advance Notification Program to better inform our patients and healthcare providers. The Foundation will continue urging UnitedHealthcare to create policies that are in the best interest of patients and will not overburden healthcare professionals.”