Proctocolectomy and Colectomy
It is common to have many questions and concerns when you are recommended for a proctocolectomy or colectomy. Our resources can help you understand each surgery and provide you with information to discuss with your loved ones, as well as with your healthcare team.
The colon and/or rectum may need to be removed in some patients with extensive disease or complications.
-
A proctocolectomy is the surgical removal of the colon and rectum.
-
A colectomy is the surgical removal of the colon.
While these surgeries may alleviate your Crohn’s disease symptoms, they require permanently altering the path of your gastrointestinal tract.
Colectomy
Your doctor may recommend this surgery if your colon is diseased and must be entirely removed, but your rectum is unaffected by Crohn’s disease.
-
Once your colon is removed, your surgeon will join the ileum, or the lower part of your small intestine, to the rectum.
-
A colectomy allows you to continue to pass stool through your anus without the need for an external pouch.
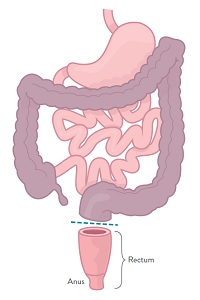
Proctocolectomy
Your doctor may recommend a proctocolectomy if your colon and your rectum (together known as the large intestine) are diseased and must be removed.
There are variations of this procedure, but patients with Crohn’s disease are generally recommended for a proctocolectomy with end ileostomy.
In an end ileostomy, the end of the small intestine is inverted through a small hole made in the abdominal wall (stoma) to divert waste into an ostomy bag.
Patients with ulcerative colitis may have the option to undergo a proctocolectomy with ileal pouch-anal anastomosis, which creates an internal j-pouch using the end of the small intestine and eliminates the need to permanently wear an ostomy bag. That procedure, however, is generally not recommended for patients with Crohn’s disease because the disease frequently recurs in the internal pouch.
What You Should Know About Proctocolectomy
-
Your colon, rectum, and anus will be removed and an end ileostomy will be created.
-
The ileum will be brought through a hole in your abdominal wall called a stoma, which allows waste to drain out of your body.
-
The stoma will be about the size of a quarter and protrude slightly from your abdomen. A healthy stoma is pinkish in color, and appears moist and shiny.
-
An external ostomy pouching system will attach to the stoma and be worn at all times to collect waste.
-
The typical site for an ileostomy is the lower abdomen to the right of the navel, just below the belt line.
-
Some patients may still feel as if they need to have a bowel movement after their surgery, just as people who have lost a limb sometimes still feel as if the limb is still there. This called phantom rectum and it is completely normal. It does not require any treatment and often subsides over time.
Living with an Ileostomy
You can live a long, active, and productive life with an ileostomy. In many cases, ileostomy patients can participate in the same activities they did before the surgery, including sports, outdoor activities, swimming and other watersports, travel, and work.
It is common for patients to initially feel self-conscious about their ostomy bag and you may notice a change in how you feel about your body image. We can assure you that the bag lays fairly flat under your clothing and is not visible to others. No one needs to know that you have an ostomy bag unless you choose to tell them.
Remember, it is just as important to take care of your mental and emotional health as it is your physical health. Speak with your doctor or a mental health professional if you feel you are experiencing symptoms of depression or anxiety.
We can help you learn how an ostomy pouching system works and guide you through some of the most common challenges of living with an ileostomy.
-
The ostomy bag is one component of a pouching system that also includes a skin barrier. You will need to empty the pouch several times a day.
-
There are several pouching systems for you to choose from. You will learn how to use your system as well as how to care for the skin surrounding the stoma.
-
You will not have any specific dietary restrictions with an ileostomy, but it is important for you to drink plenty of fluids to avoid dehydration and loss of electrolytes.
-
Eating foods high in pectin, including applesauce, bananas, and peanut butter, will help thicken your stool output and control diarrhea.
Potential Ileostomy Complications
The small intestine may become obstructed from food or scar tissue. If food is obstructing your intestine, it should be temporary until the food moves through your intestines.
Notify your doctor or other health care provider immediately if you experience these symptoms:
-
Infection from the surgery or at the site of the stoma
-
If your stoma is protruding more than normal outside of your abdominal wall, called prolapse, or retracting further inside your body, called retraction.
-
If no waste material exits the stoma for four to six hours and is accompanied by cramps and/or nausea, which could indicate a blockage
Sex After Proctocolectomy
It is normal to be worried about how an ileostomy will impact your sexual activity. Most people find that their sexual function is not impaired in the long-term.
-
Some men may experience erectile dysfunction and some women may notice pain during intercourse, but these complications are usually only temporary.
-
You and your partner may need to make some adjustments to accommodate the presence of an ostomy pouch.
-
The United Ostomy Associations of America offers a helpful guide on intimacy and sexuality with an ostomy.
Ask Your Doctor
-
What preparations will I need to make before my proctocolectomy or colectomy?
-
What are the potential complications from surgery?
-
Will my ostomy be temporary or permanent?
-
What kind of restrictions will I have after my surgery?
-
How long will it take me to recover from my proctocolectomy or colectomy?
-
How will the surgery affect my diet and bowel movements?
-
How and when will I learn how to care for and clean my ostomy and stoma?
-
What supplies will I need at home?
-
Will I need additional surgeries?