How is IBD Diagnosed?
The path to receiving a Crohn’s disease or ulcerative colitis diagnosis can be overwhelming. We can help you understand the process of diagnosing inflammatory bowel disease (IBD), and the common tests and procedures your healthcare team may recommend so that you are educated and prepared.
No single test can confirm a Crohn’s or colitis diagnosis. Your healthcare team will evaluate your current medical history and use information obtained from diagnostic testing (tests used to help diagnose a disease or condition) to exclude other potential causes of your symptoms, since gastrointestinal symptoms are common and can have a variety of causes. Getting the right diagnosis may take time, but here is some helpful information and tips to better understand the testing and diagnostic process.
Initial testing | Blood and stool lab tests | Endoscopy
Radiology/diagnostic imaging | Prognostic testing
Initial testing and evaluation
The first step to getting an IBD diagnosis and starting treatment involves your healthcare team obtaining a thorough medical history from you and performing a physical exam of your body. Your doctor will ask questions about your overall health, diet and nutrition, family history, and your daily routine in order to get a sense of your overall health and well-being.
Helpful tips:
- Share with your doctor any previous medical records including summaries of visits with other doctors, lab results, and other tests that may have already been performed. You may need to sign a release form from one office before records can be sent to another office. Please allow enough time to have the records sent.
- You may want to bring a trusted family member or close friend to your appointment to help make the experience less stressful and help you remember information from your visit. You may also want to bring a notepad to take notes on the order of next steps you may need to take in your care.
- Write down questions and your timeline of symptoms beforehand and bring the list with you to your appointments, so you don’t have to worry about forgetting anything important.
- Contact your insurance to understand your coverage and potential out-of-pocket costs for the diagnostic process. Each insurer is different, so your doctor may not know which tests your insurance will cover.
- Check out our IBD testing discussion guide which lists common tests and procedures your healthcare team may recommend and follow-up questions you can ask.
What tests are used to diagnose IBD?
- Your first tests will likely include blood and stool laboratory tests.
- Further testing could include imaging studies of your gastrointestinal (GI) tract. Your doctor may recommend a test that uses a contrast agent (oral or intravenous) that allows for a clearer and more detailed picture of your GI tract.
- Additional testing may include looking inside your GI tract through an endoscope.
These tests are explained in greater detail below.
Blood and stool laboratory tests
Doctors commonly use blood and stool tests as part of your initial diagnostic work-up. Proteins found in blood and stool, also called biomarkers, during blood and stool tests may be useful for detecting inflammation. Although these tests will not reveal what’s causing the inflammation, they may indicate that further testing is needed to identify where the inflammation is coming from. Specific biomarker levels may also be followed over time to help assure that the therapy being used is optimized and that your inflammation is truly controlled.
Blood biomarkers include c-reactive protein (CRP) and erythrocyte sedimentation rate (ESR), both of which help detect the presence of inflammation in the body.
Fecal biomarkers include calprotectin and lactoferrin, both of which are proteins found in stool that can indicate gastrointestinal inflammation.
Blood tests involve a blood draw from a vein in your arm. Stool tests involve utilizing a stool collection kit provided by your doctor or the lab along with specific instructions on how to collect a sample.
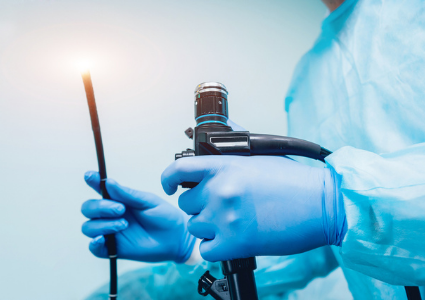
Endoscopy
After reviewing your blood and stool test results, your doctor may recommend additional tests to look inside your GI tract. While these tests are more invasive, they are extremely important, and your healthcare team will be careful to minimize any discomfort.
Your doctor may recommend an endoscopy – an outpatient procedure during which a small camera mounted to the end of a lighted tube is used to look inside your GI tract. An endoscopy helps your physician see if inflammation is present, where it is located, assess its severity, and obtain tissue samples (biopsies) to confirm your diagnosis. Endoscopies can also be used to help monitor whether your treatment is working. Healing of the lining of the intestine (mucosal healing is a sign that your treatment is helping and can be seen during an endoscopy.
Certain endoscopies, like colonoscopies, require bowel preparation the day before the procedure. Before your test, you will typically drink a laxative that removes stool and debris from your intestines resulting in diarrhea. Make sure you follow the directions from the pharmacy closely. Bowel preparation can take some time and can be uncomfortable; however, the result will be a clean intestine, which will make it much easier for your doctor to view your intestinal lining. We encourage you to your healthcare team about ways to prepare and tips for making those steps easier.
Endoscopies used in IBD testing include:
- A colonoscopy allows doctors to examine the colon, or large intestine, by inserting a flexible, lighted tube through the opening to your anus. The tube runs through the entire length of the colon and the end of the small intestine (terminal ileum). Typically, you will receive sedation prior to the procedure to minimize discomfort.
- An upper GI endoscopy allows doctors to see the GI tract from the top down using a flexible, lighted tube that’s inserted through your mouth, down the esophagus, into your stomach, and can go as far down as the duodenum (the first section of your small intestine). It is used in suspected or diagnosed Crohn’s disease cases to evaluate different symptoms. These symptoms can include, but are not limited to, upper abdominal pain, nausea, vomiting, and difficulty swallowing. You will receive a sedative throughout the procedure to minimize discomfort.
- A sigmoidoscopy allows doctors to examine the left side of the colon or rectum by inserting a flexible, lighted tube through the opening to your anus. A sigmoidoscopy can be a good diagnostic test to confirm ulcerative colitis and to monitor your response to therapy. Because the procedure is very brief, it can often be performed without a sedative and is associated with less discomfort than a colonoscopy.
- A pouchoscopy is an exam used to evaluate the ileal (small bowel) pouch (commonly called a j-pouch) created after colon surgery for ulcerative colitis.
- A video capsule endoscopy is performed by swallowing a small, pill-sized camera, which takes pictures of your small intestine and bowel as it travels through your GI tract over the course of 8 to 12 hours. These pictures are stored in a recorder that you wear from the time you swallow the camera until the study is complete. At the end of the test, you will return the recorder to your doctor. The camera does not have to be removed by a doctor, because it is later released when you pass a bowel movement.
Biopsy
Your doctor may take biopsies of your colon or other areas of your GI tract while performing a colonoscopy or endoscopy. During the biopsy, a small piece of tissue is removed from the inside of the intestine.
- Your biopsied tissue will be analyzed (reviewed) in a laboratory and screened for any features that help make the diagnosis of IBD or any abnormal cells (pre-cancerous or cancerous) in the inflamed area of the intestine.
- While a biopsy sounds scary, medical advances have made this procedure virtually pain-free.
- After a biopsy, you may experience a little blood in your stool and that is normal.
Chromoendoscopy
Your doctor may want to use a chromoendoscopy during a colonoscopy. A chromoendoscopy involves spraying a blue liquid dye into the colon to highlight and detect slight changes in the lining of your intestine, such as polyps (small clumps of cells). Polyps can then be removed and/or biopsied. It is common to have blue bowel movements following this procedure.
Radiology scans or diagnostic imaging
Traditional upper GI endoscopy and colonoscopy are not be able to reach about two-thirds of the small intestine. Therefore, in addition to capsule endoscopy, various radiologic exams or diagnostic imaging may be performed to evaluate these parts of the intestines as well as to evaluate the actual wall of the bowel and surrounding areas outside the bowel.
X-rays
X-rays are the oldest way of imaging the inside of the body. X-rays are cost-effective and useful for detection of blockages in the small or large intestine.
Barium contrast studies
During a barium study, you will ingest a contrast material (barium) and have images taken with traditional X-ray technology. Barium is a chalky/milky liquid that you drink prior to the procedure. A series of X-rays are taken to observe the material flowing through the digestive system. These studies include:
Upper GI series examines the esophagus, stomach, and first part of the small bowel (duodenum) for patients with Crohn’s disease
Small bowel series and small bowel enteroclysis examines the entire small bowel. For a small bowel series, you will drink several cups of barium, and then have an X-ray taken every 15–30 minutes as the barium travels down the small intestine and enters the large intestine. The time required varies but may take four to five hours. An enteroclysis is similar, except that the barium is placed directly into the small intestine through a tube introduced into the GI tract via the nose or mouth.
Lower GI series involves inserting the contrast material directly into the rectum (barium enema) and provides images of the colon or large intestine. During the exam, the colon is distended with air to provide better images.
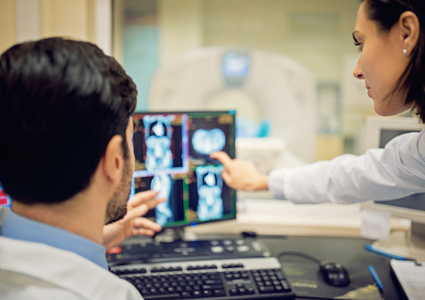
Cross-sectional imaging
Cross-sectional imaging is comprised of computed tomography scanning (CT scan) and magnetic resonance imaging (MRI). These techniques are extremely helpful in diagnosing and managing IBD. They can evaluate the thickness of the bowel wall and can detect inflammation and complications, such as fistulas, abscesses, and obstructions.
CT scan, also known as a CAT scan, takes simultaneous X-rays from several different angles to reconstruct a realistic image of the internal organs. The CT scan is used to rule out complications of IBD, such as intra-abdominal abscesses, strictures, small bowel obstructions or blockages, fistulas, and bowel perforation. This will usually involve the use of oral and intravenous contrast.
CT enterography (CTE) is a specific type of CT scan. During this exam, a special oral and/or intravenous contrast agent is given to better visualize the intestines. In addition, CTE reconstructs images in 3D to better visualize the small bowel in relation to other organs. Your doctor may suggest this exam to identify areas of inflamed bowel and more subtle obstructions or blockages.
Magnetic resonance enterography (MRE) is a special MRI study that looks more closely at the small intestine. An MRE is different than the CTE because it doesn’t involve radiation. During the MRE, you will be asked to drink contrast that helps expand the small intestine. You will also be given a contrast agent through an IV. The oral and IV contrast help determine if inflammation or changes are old versus new, if intestinal narrowing (stricture) is present, if abnormal connections (fistulas) are present, or if there are abscesses. The MRE can also help clarify the length, extent, and severity of small bowel disease.
Magnetic resonance cholangiopancreatography (MRCP)is a specialized MRI exam that provides a view of the bile ducts, gall bladder, liver, and pancreas. This test is helpful in diagnosing conditions such as primary sclerosing cholangitis (PSC), a condition that involves inflammation and scarring in the bile ducts which are located both inside and outside of the liver.
Prognostic testing
Researchers are currently studying biological products found in a person’s blood, tissue, or other body fluids to assess if they can be used (along with other individual factors such as diagnosis, age, and location of disease) to help predict the progression of IBD. These studies are known as prognostic testing.
Whereas diagnostic tests help confirm the diagnosis of IBD, prognostic tests can help predict whether you may experience a mild or severe case of IBD or if you are likely to develop complications down the road. Prognostic testing allows physicians to identify patients who may benefit from more aggressive early treatment. They also help predict the likelihood of repetition of disease or if a patient is more likely to have a response to a particular medication. Prognostic testing allows for more personalized, individualized treatment.
Prognostic testing offers some challenges. Many clinicians and researchers feel that more data is needed to truly understand who to test and when and how to use this information to improve outcomes. In addition, many of these tests are expensive and may not be covered by insurance so you may want to have a discussion with your insurance carrier to check coverage of costs.
The following is a list of prognostic tests that are currently available to IBD patients in the United States. These tests have not been widely adopted in clinical practice due in part to the need for more definitive evidence that the results are helpful in making clinical decisions. It is the Foundation’s hope that as research continues, more patients will benefit from this type of test and be able to make effective, early treatment decisions to improve their health outcomes.
Please note: The Foundation does not specifically endorse these tests and is providing this list for education and informational purposes only.
The Foundation is committed to accelerating research focused on the identification and validation of biomarkers of inflammation and on developing new technologies to detect these biomarkers. Learn more about the Foundation’s commitment to biomarker research and prognostic testing.
This program is generously supported, in part, by: