If your doctor has told you that you need to have ostomy surgery, you might feel overwhelmed and have questions. Ostomy surgery is commonly performed in patients with Crohn’s disease or ulcerative colitis, and it can provide a new lease on life—a life with fewer hospitalizations and less pain.
So, what exactly is ostomy surgery? Ostomy surgery is a procedure that allows stool to pass through a surgically created opening in the body (a stoma) to discharge bodily waste. Your stoma is the part of the bowel (small or large intestine) that pokes out of your abdominal wall and provides an opening for waste to pass out of. The waste is then collected from your stoma into an external ostomy pouch (i.e., a bag) or appliance which is adhered to your abdomen on the outside of your body.
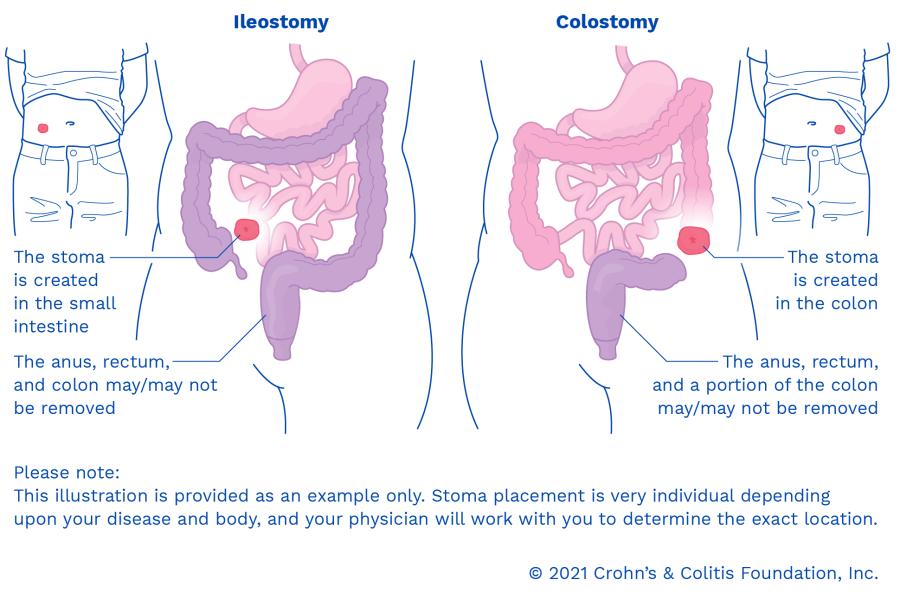
There are two common types of ostomies for IBD patients named for the part of the intestine that is opened. An ileostomy is an opening from part of the small intestine (called the ileum) and a colostomy is an opening from part of the large intestine (colon). Your ostomy may or may not be permanent, but recovery from surgery will be similar.
Your ostomy care team
Before and after your surgery, you will have an ostomy care team that helps teach you how to care for your ostomy. This will consist of your gastroenterologist, surgeon, and healthcare professionals specializing in ostomy care. An ostomy management specialist (OMS) is a healthcare professional who completed a board certification in ostomy management. Wound, ostomy, and continence care nurses (WOCN) specialize in the treatment of skin, unhealed and chronic wounds, ostomies, and ulcers. These specialists, along with your healthcare team, will help teach you how to care for your ostomy. They will answer your questions, provide training, and give you an overview of the supplies you or your child may need.
Post-operative tips
It’s important to talk to your healthcare team about what you can expect post-surgery. Immediately following ostomy surgery, patients can experience output as high as 1.5 liters a day. As time passes, the output will decrease as the ileum picks up some of the fluid and electrolyte absorption previously done by the colon. It is important to stay hydrated. The majority of readmission is due to dehydration; therefore, it is very important to drink rehydration fluids (containing sodium, glucose, and amino acids). Always call your provider if you have an abrupt decrease in output, concerns about obstruction, or experience pain or a new protrusion.
Recovering from ostomy surgery may take some time - be patient with your progress! Below are some helpful tips and tricks from healthcare providers and fellow IBD ostomy patients to help in your day-to-day life, as well as planning for special occasions.
Jump to:
Caring for your ostomy | Living with an ostomy | Emotional health
Parents, kids, and teens | Helpful resources
Caring for your ostomy
After ostomy surgery, you will work with your care team to learn how to care for your ostomy. This will include understanding how to change your ostomy appliance, care for the skin around your stoma, avoid leaks, manage your output, manage odor, and more.
-
Changing your Appliance
-
After ostomy surgery, you will work with your care team to learn how to care for your ostomy. This will include understanding how to change your ostomy appliance, care for the skin around your stoma, avoid leaks, manage your output, manage odor, and more.
Ostomy appliances consist of a few parts:
-
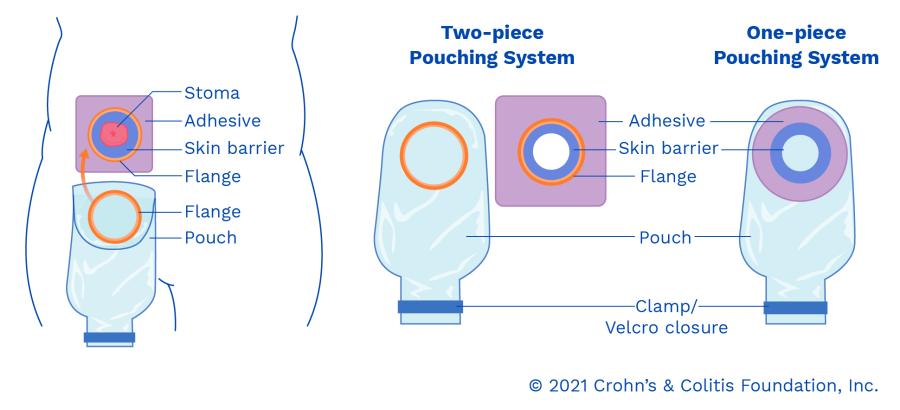
The flange (also known as a face plate, wafer, or skin barrier) is what secures the pouch to the abdominal wall. The flange adheres to the skin around the stoma and protects the skin from irritation from the stool output.
Ideally, your appliance will remain attached to your abdomen for approximately 3-7 days (known as your wear time). Your appliance is emptied approximately 4-5 times daily. You should empty your bag regularly and avoid waiting until it is completely full, which can cause the pouch to get heavy and loosen the seal, potentially causing a leak. Remember, everyone’s body type and skin are different and everyone can have different wear times.
Ostomy appliances vary based on what type of surgery was done. In general, ostomy appliances come as either one piece (where the pouch and the flange are connected permanently) or a two-piece appliance (where the flange and the pouch can be separated allowing the patient to change the pouch without changing the flange).
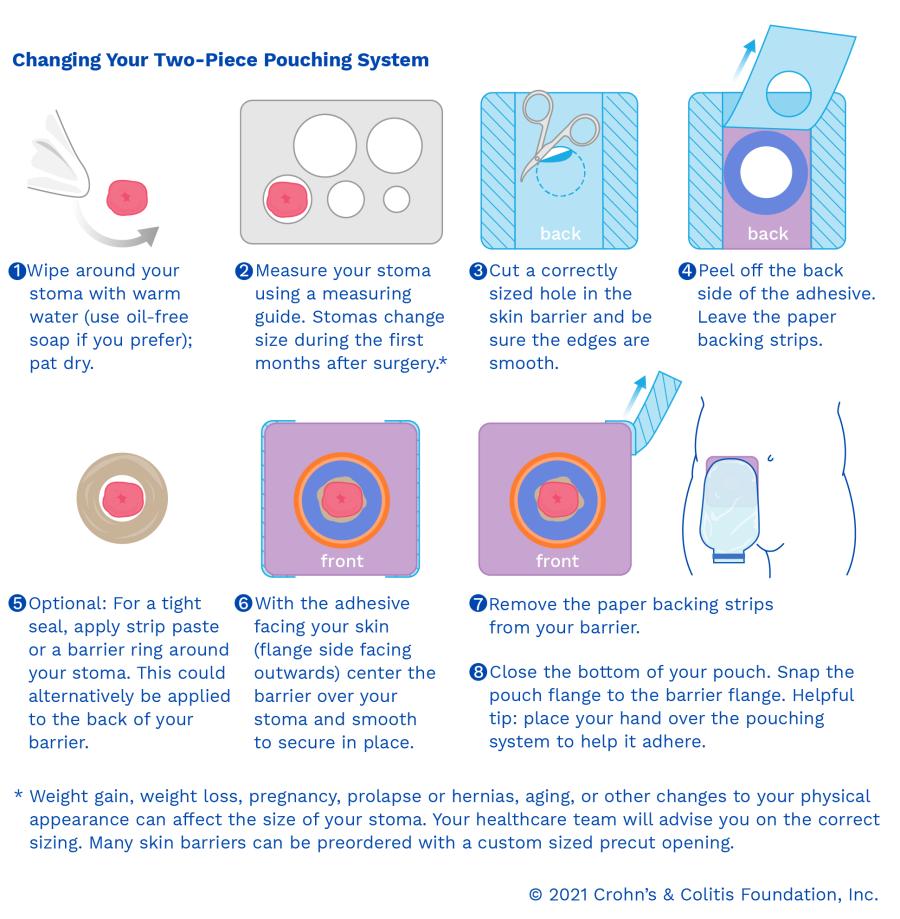
Following your surgery, your OMS will help you understand the different types of pouching systems, select the best type for you, and explain all the steps of changing your pouch. It’s always a good habit to wash your hands properly prior to and after handling any of your appliance parts. When you remove the one-piece system, or the flange, gently peel it away from your skin – starting at the top and working downward while pressing against your surrounding skin. You can use an adhesive remover to help peel away the flange. After the flange is off, inspect your skin for any breakdown (redness, rash or change in color), clean and dry the area, and apply a new flange. When the change is complete, a good tip is to hold your hand over the pouch, for a few minutes, to help the barrier of the flange to adhere to the skin.
-
Skincare
-
It’s important to take special care of the skin around your stoma. It should look like the skin anywhere else around your abdomen; however, over time though, the skin around your stoma might appear darker or lighter – and this is normal. Water should be all you need to clean the skin; but, if you would like to use soap, be sure to use a very mild cleanser with no oils or scents. A small amount of bleeding can happen if you brush up against the stoma – this is also normal. This occurs because the lining of the intestine – what your stoma is made from – can be fragile (similarly to when you brush your gums).
-
Avoid using lotion, cream, powder, wipes, ointments, or rubbing alcohol around your stoma unless advised by your healthcare team as that can impact the application of the skin barrier
-
If you experience irritation, rash, redness, or broken skin, reach out to a qualified health professional like a WOCN
-
Avoiding leaks
-
You want to feel secure in your pouching system and enjoy your life without worrying about having a leak. However, leaks can happen and can be caused by skin irritation, sweat/excess water underneath the barrier, too much gas in pouch, or from a pouch being too full.
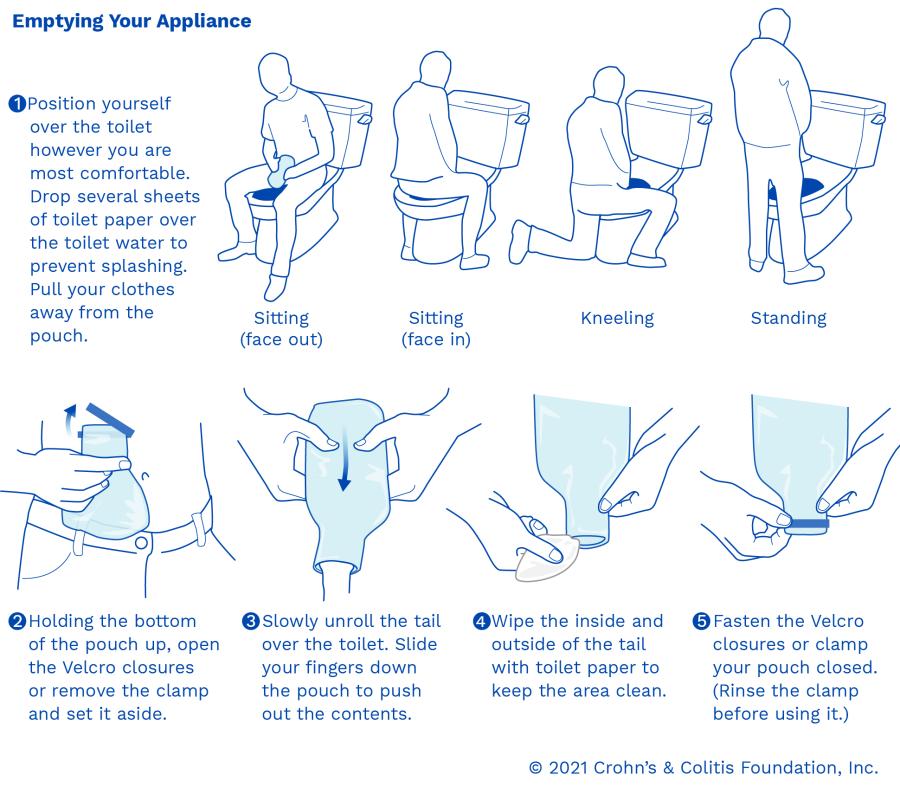
It’s a good idea to empty your pouch regularly (when it’s a third to halfway full) and before you change your appliance. Some people prefer emptying their pouch at a set time in the day, such as first thing in the morning. You want to avoid waiting until it is completely full, which can cause the pouch to get heavy and loosen the seal.
Here are some helpful tips to avoid leaks:
-
A skin barrier ring or paste can be used with the flange as extra protection to ensure your pouch fits properly around the stoma
-
When removing your flange, gently peel it away from the skin, starting at the top and working downward while pressing against surrounding skin
-
Change your one-piece system or flange on a regular basis
-
Managing high output
-
Your output (stool) volume and consistency will depend on the type of ostomy you have, and it is important to understand when your output is too high. The function of the colon is to absorb fluid and electrolytes from the stool. In the immediate post-operative period following removal of the colon (colectomy), the ileostomy stool output can be as high as more than 1.5 liters per day. Generally, the goal for stoma output is between 800 and 1,200 ml in 24 hours period. For children, output is assessed by their current weight, so it’s best to talk to your child’s doctor if you have any concerns. Active disease/flaring, high sugar intake, infection (such as Clostridiodes difficile or C. diff), or short bowel syndrome can be some causes of high output.
If you are experiencing higher than normal output – here are some dietary considerations:
If you think you may be experiencing high output, talk to your healthcare provider about your options, such as an anti-diarrheal or prescription medication.
-
Odor control
-
Ostomy appliances are air-tight, and you should only notice odors when changing or emptying your pouching system. Should you notice an odor, this may be a sign that leakage is about to occur. If you are concerned about preventing odor, you can consider the following:
-
Monitor your body’s response to food and beverages as certain items may cause an increase of gas in your bag. Asparagus, beer, broccoli, fish, garlic, and many fatty or processed foods all may cause odor.
Living with an ostomy
Adjusting to your new normal - life with an ostomy - will take some time. You will likely notice a drastic improvement in how you feel immediately, but it's important that you take time to learn your new body and the adjustments you need to make in your daily life.
Video Length
00:01:44
Living with an Ostomy: Shawn
Video Length
00:01:37
Living with an Ostomy: Abby
Video Length
00:01:50
Living with an Ostomy: Shaun
-
Eating
-
Immediately following your surgery, eating a diet that's low in insoluble fiber, low in fat, and low in added sugars may help your GI tract to rest and heal. This includes foods that are easier to digest, produce less gas, and help minimize cramping, diarrhea, and potential obstruction. It is important to maintain this diet for four-to-six weeks after surgery and talk with your doctor about when to return to adding new foods. Click here for more detailed information on diet, nutrition, and IBD.
Here are some general guidelines for eating with an ostomy:
-
Avoid foods that are difficult to break down due to their tough texture as they may cause a blockage/obstruction. Some examples include celery, grapes, raisins, cruciferous vegetables, and mushrooms. Also, slowly increase the number of fiber-containing foods (fruits, vegetables, whole grains, beans, whole nuts, raw seeds) in your diet to help prevent obstructions. Click here for more information on blockages/obstructions.
-
Replace fried/greasy foods with low fat alternatives, such as air fried or baked foods. Choose lean sources of protein, like poultry, fish, eggs, smooth nut butters, and tofu, more often as these tend to be better tolerated.
-
Avoid sugar alcohols (sorbitol, mannitol, etc.), artificial sweeteners, and highly sugary foods and beverages (soda, ice cream, cake, etc.) as they may increase output
-
Add foods that tend to thicken up stool, such as bananas, oatmeal, peeled potatoes, rice, bread, pasta, applesauce, creamy peanut butter, or chia seed pudding, to all your meals
-
Clothing
-
There is no need for any special ostomy clothing – wear whatever you are comfortable in! Some patients find that tights or leggings add extra support and that even high waisted pants feel more comfortable but that is entirely up to you. There is also intimate attire made especially for ostomates that some find helpful.
-
Bathing and showering
-
Water does not impact your stoma – so you can bathe or shower with your pouch on or off. If you do leave your pouch off, just be sure your skin is entirely dry before putting on your new appliance as it will only stick to dry skin.
-
Exercise and sports
-
If you are just starting or getting back into exercise after surgery, always consult with your healthcare provider and start slowly. You may want to consider wearing supportive clothing or a stoma guard to keep your pouch in place.
Worried about sweating when you exercise? If you pouch fits properly, it should not irritate your skin. However, certain exercises or activities may cause more sweat (hot yoga, outdoor sports in hot/muggy weather) and you may want to consider ostomy wraps or guards to provide more security when doing these activities. Don’t worry about swimming – swimming is safe and having an ostomy shouldn’t keep you from beach activities or a dip in the swimming pool. Your ostomy pouch is water resistant and is designed not to leak. If you have output concerns, eat a few hours before swimming and empty your pouch just before going in the pool.
-
Travel
-
When you are heading out of town, it’s important to pack extra supplies. If you are traveling on an airplane, pack your supplies in at least two places (in your carry-on bag AND your checked bag) just in case you have a delay with your baggage. If you use scissors to cut your skin barriers, they are allowed in your bags if they are no longer than 4 inches. However, you may want to consider pre-cutting your barriers before traveling to avoid having to pack scissors. One helpful hint with air travel - prior to take off ensure that you have released all the gas out of your pouch because changes in air pressure can cause the pouch to expand.
If you have concerns about screenings and pat-downs, you can request a private screening for you and a travel companion. You can also pack documentation that easily communicates the necessity of your ostomy and accompanying supplies. You should not be asked to expose your ostomy or remove clothing in sensitive areas. You can always request to speak with a Supervisory TSA Officer about any concerns you may have. Click here for a helpful travel communication card.
-
Intimacy
-
After surgery, you may experience some physical and emotional changes that can have a direct impact on your sexual functioning and body image. Men may experience erectile dysfunction and women may notice pain during intercourse. These conditions are usually only temporary. Talking to your partner is key to strengthen your intimate relationship and communicate your needs. You and your partner may need to make some adjustments to accommodate the presence of a pouch, but your partner will take the cue from you. You may consider securing your pouch with an ostomy wrap. Always share your physical limitations, pain (if present), fears, and what you enjoy and do not enjoy. To have a positive relationship with any partner, it is critical to accept your body –that is the key towards others accepting it as well. Having an ostomy does not mean you need to ignore your sexuality. For more information about sex, intimacy, and IBD, check out our fact sheet. For more information on intimacy with an ostomy, visit www.ostomy.org/sexuality.
-
Fertility, pregnancy, and delivery
-
It is important to talk to your doctor before trying to become pregnant. Although your underlying surgery may affect fertility and ability to get pregnant, the presence of a stoma does not and should not deter one from getting pregnant. Every IBD patient is different; however, it is safe to get pregnant with an ostomy and generally ostomy patients do well with pregnancy if there are no other health issues.
During pregnancy, your stoma size may increase but it will return to normal after delivery. You may need to use different products or adjust the size of your flange when you change your appliance. Your stoma may also fall out of view as your pregnant stomach grows, so using a mirror or having a partner help you change the appliance is recommended.
Your care team may recommend that you have a surgeon on-call during delivery; however the presence of a stoma does not prevent vaginal delivery.
-
At the workplace
-
You may be wondering how adjusting to life with an ostomy will affect you at work. Generally, once you have recovered from your surgery, you should not have any limitations doing your job. It’s best to talk about your return to work with your healthcare provider as this will depend on your comfort level, work environment, and how physical your job is.
Here are some tips for managing your ostomy at work:
-
It’s up to you if you want to tell your employer or co-workers about your ostomy. However, if you require certain accommodations, such as access to a different bathroom or frequent breaks, you may need to have a conversation with human resources.
Emotional health
Video Length
00:47:34
Ostomies and Caring for your Mental Health
Ostomy awareness day 2022 - mental health
Having ostomy surgery can be life changing. For some, it may seem devastating, but for others it may bring a sense of relief. It’s normal for ostomy patients to experience concerns about self-care, self-esteem, body image, relationships, work, and daily life after surgery. It’s important to check in with yourself about how you are feeling and seek help when needed. Here are some tips on managing your emotional health when planning for ostomy surgery:
For parents, kids, and teens
Child and caregiver tips
As a parent, you may have a lot of questions and concerns about how to support your child as they get used to life with an ostomy. Learning as much you can about your child’s ostomy is the best way to support them during this life change. Ostomy surgery can be difficult for your child and family members to adjust to. Here are some ways you can show your support as a caregiver:
-
Be open: Your child may not want to discuss their ostomy with everyone around them, and that’s okay. However, it’s important to guide open conversations around them about their ostomy to encourage them to feel comfortable asking questions or raising concerns when needed.
-
Be understanding: Children who undergo ostomy surgery may have additional physical needs temporarily, such as pain control and adjusting to a stoma, and it important to listen to how they are feeling. The calmer and more accepting you are about the stoma, the easier it will be for your child to accept it.
-
For teenagers: Adolescence can already be a difficult time due to puberty and body image issues, and an ostomy can cause additional stress for teens. It’s important to check in with your teen regularly to see how they are adjusting and discuss mental health concerns with your teen’s healthcare team. Click here for more information about mental health and teens with IBD.
Children and teens with ostomies may need certain accommodations at school, like having the ability to store extra supplies, access to a specific bathroom, or extra time to change their appliance during school hours. For more information about planning with your child, see Taking IBD to School.
|
|
Hear from others:
“I had my ostomy surgery as a child. One thing that my parents did for me that was extremely helpful was related to school. Every year my mom would go in and talk to all of the staff. She also got it set up to where I could use the staff's restroom for when I needed to go to the bathroom or change my bag. This relieved so much stress for me.”
-Megan, IBD Patient
|
College students
As a college student with an ostomy, you may have questions about how to handle class schedules, activities, living on campus, and more. It’s important to schedule a meeting with your school’s health center before arriving or returning to campus to make sure they are aware of your ostomy and your needs. You don’t need to tell everyone about your ostomy, but it may be helpful to tell certain teachers or housing directors as you may be able to receive certain accommodations and get the support you need. Click here for more information about support services and accommodations at school.
Hear from others:
“I enrolled in a full-time MBA while I had my ostomy. I had conversations with my professors at the beginning of each semester, letting them know that there would be times when I would need to quietly excuse myself from class due to a health issue. They did not ask any further questions but were happy that I let them know."
-Anthony, IBD patient
|
|
Helpful resources
United Ostomy Associations of America, Inc.
A (501)(c)(3) non profit organization that supports, empowers, and advocates for people who have had or who will have ostomy or continent diversion surgery.
https://www.ostomy.org
Grateful Patient Foundation/Alive & Kicking
Education, support, and community resources for ostomy patients
https://www.ostomyrecovery.org/
This program is generously supported, in part, by Hollister
This project was created in partnership with:
Thank you to our content reviewers and contributors:
George Salamy, Richard Rood, MD, and The Crohn’s & Colitis Foundation’s Ostomy Workgroup