What to do if Denied Coverage
I just received a denial, what happens now?
Receiving a coverage denial notice for yourself or your loved one can be stressful, frustrating, time-consuming, and complicated. The first step in managing the denial process is to understand the reason for the denial so you can take steps to try to appeal and resolve it. To help navigate the process, below are some tips on denials, appeals, and where to find more information.
What are some common reason for denials?
If you received or used a medication or service, it is important to review the Explanation of Benefits (EOB), a document from your insurance company that provides information about your claims, to identify the reasoning behind the denial. If you were denied prior to receiving a medication or service, you should review the denial letter for the specific reason(s). If you are unsure of the reason for denial, contact your insurance company or healthcare team for an explanation.
Some common reasons medications are denied include:
- There may have been a process error: examples include a missing authorization code, the paperwork was not filed in a timely manner, or a payment was not received.
- There are limits on the amount of medication (dose, quantity, or intervals between doses) you can receive.
- The insurance company has a medication formulary (a list of medications that it covers) that prefers you use a generic or biosimilar medication rather than the prescribed brand name medication.
- The medication is non-formulary, meaning it is not covered by your insurance plan.
- A pre-authorization is required by your insurance company prior to receiving the medication.
- The insurance company requires you to try and fail another medication(s) first before providing coverage for your prescribed treatment. This is also known as step therapy or fail first.
Some common reasons procedures and testing may be denied include:
- There may have been a process error: examples include a missing authorization code, the paperwork was not filed in a timely manner, or a payment was not received.
- The procedure/test is not a covered benefit under your insurance plan.
- The provider completing the procedure is not in network for your insurance plan.
- The services are considered investigational or not recognized as standard medical care by your insurance company.
- A pre-approval/authorization is required prior to completion of the procedure or test.
Appealing a Denial
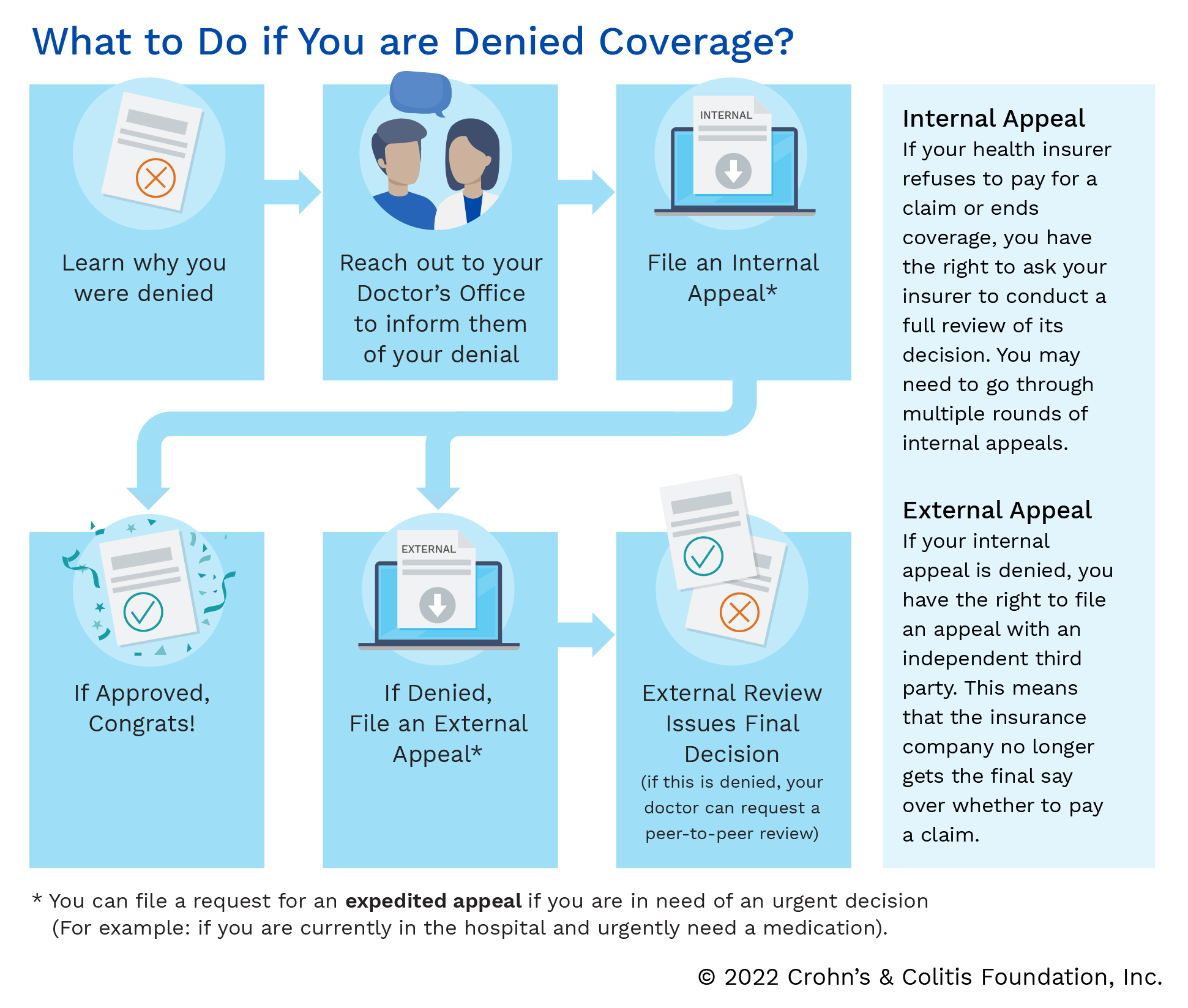
When you file an appeal, you are asking your insurance company to reconsider its decision of denying coverage for a specific medication, treatment, or service. Depending on your insurance plan, there may be a deadline for filing an appeal, so pay attention to timelines for submission. Most of the time, your doctor's office will handle submitting an appeal, but patients have the option to submit an appeal letter as well. Contact your healthcare team for support when writing your appeal letter, as they may have templates or helpful information to include. After you submit, follow up with your insurance company and confirm they received your appeal letter and that the appeal is being processed.
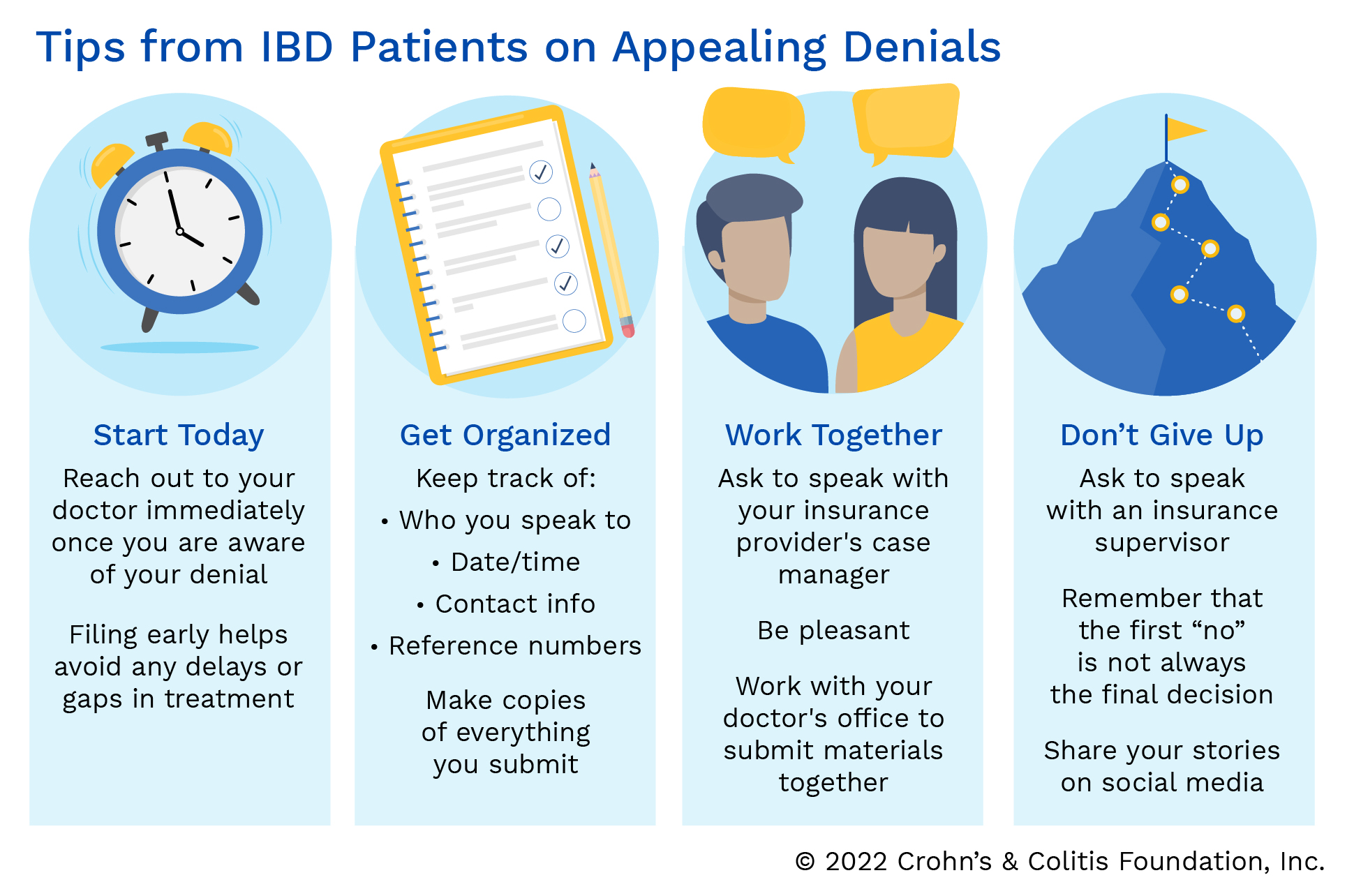
Helpful tips when writing an appeal letter
The Crohn's & Colitis Foundation offers a variety of sample letters/templates you can download and customize to help with your appeal. When writing your appeal letter, clearly state the purpose is to appeal a decision. Include the policy number, claim number, date of service, and your completed contact information (home address, best phone number, and email address). Be as concise as possible, and include only facts related to the denial reason. Check for spelling and grammar errors. You want to include a letter(s) from your healthcare team documenting your personal IBD journey and showing medical necessity for the denied medication, treatment, or service, as well as copies of any relevant medical records.
When sending your letter, be sure to include any of the items below as supportive documentation:
- A copy of the denial letter or Explanation of Benefits (EOB).
- A copy of any bills received (if applicable).
- A copy of the completed appeal form from the insurance company.
- If needed, an 'Appointment of Representative' Form which allows you to name someone to make medical decisions for you.
- Letter of medical necessity from your healthcare team and any other supportive letters.
- Relevant medical records related to the denial.
- Supportive peer-reviewed journal articles.
Remember:
- File appeals in a timely fashion and pay attention to deadlines - there are often short windows during which an appeal can be filed after a claim is denied.
- Keep all copies of correspondence from your gastroenterologist's office and the insurance company.
- Keep a record of all names/titles of everyone you speak to and any case or authorization numbers.
- Only send copies of documents and keep all originals on file for reference.
Medicare Appeal Process
The appeal process is different from each part of Medicare, Part A (hospital insurance), B (medical/outpatient insurance), C (Medicare Advantage Plan), or D (prescription drug plan). Denials can often be found in the Medicare Summary Notes (MSN) that shows all services and supplies that are billed during the 3-month period of the notice.
Resources:
- Medicare Beneficiary Ombudsman helps with complaints, grievances, and information requests.
- Senior Health Insurance Programs (SHIP) offers free services to help people who have Medicare questions or concerns. To find local Medicare help visit SHIP.
Medicaid
Medicaid appeal rights are established federally, but each state has its own individual rules for processing the appeals. For all Medicaid appeals, you must be given written notice, known as "notice of action," when denied a service or medication that you or your physician has requested.
For more information about how each state handles appeals, visit your state's Medicaid website or the local Department of Human Services.
Do I have any other options if I've exhausted my appeal rights?
- You can inquire about applying for a pharmacy exception through your insurance company. This must be filed by your physician.
- If your employer health insurance is a self-funded plan and you decide to disclose health information, your employer can make a compassionate appeal directly to your company's top executives and ask them to make the final decision and approve treatment.
- Reach out to your elected officials, file a complaint with the state department of insurance, or voice your concerns on social media, tagging your insurance company and other relevant people.
- Reach out to your state's Consumer Assistance Program (CAP) or Department of Insurance: https://www.healthcare.gov/appeal-insurance-company-decision/external-review
- Reach out to Jennifer Jaff Careline for case management support and patient advocacy services.
- Apply for patient assistance for a prescribed medication, charity care at a hospital, facility, or healthcare office.
- If available, choose a different plan with expanded benefits during open enrollment.
